Getting Diagnosed
Finding out you have Parkinson's can be a lengthy process. Explore how a Parkinson's diagnosis is made and what type of diagnostic tools are used.

💡 Quick Summary
-
Parkinson’s disease is diagnosed clinically, based on medical history, current symptoms and a physical exam.
-
No single lab or test confirms a diagnosis, though tests like an MRI, DaTscan or blood work can help rule out other conditions.
-
Key diagnostic criteria include bradykinesia (slowness of movement) plus at least one of the following: resting tremor, stiffness/rigidity, or balance issues.
-
Advanced tools like DaTscan (images dopamine function) or the Syn-One Test (skin biopsy for PD-related proteins) can support diagnosis but are not always needed.
Parkinson’s disease (PD) is a “clinical” diagnosis. This means that an individual’s history, symptoms, and physical exam are used to make the diagnosis. There is not a specific lab or imaging test that can diagnose PD. However, certain tests such as magnetic resonance imaging of the brain (MRI brain), a dopamine transporter scan (DaT scan), or blood work can be used to support the diagnosis of PD or to rule out other medical conditions that can mimic PD.
Making an accurate diagnosis of Parkinson’s, particularly in its early stages, can be difficult. Often, an internist or family physician is the first to make a diagnosis. Many people may seek an additional opinion from a movement disorder specialist. A movement disorder specialist is a neurologist with experience and specific training in the assessment and treatment of PD and related disorders.
The newest criteria for diagnosing Parkinson’s was developed by the International Parkinson and Movement Disorder Society (MDS), and reflect the most current understanding of PD.
To consider a diagnosis of Parkinson’s disease, a person must have bradykinesia (slowness of movement). In addition to bradykinesia, a person must also have one or more of the following:
- Shaking or tremor in a limb that occurs while it is at rest
- Stiffness or rigidity of the arms, legs, or trunk
- Trouble with balance and falls
Neurology Appointment
The first and most important diagnostic tool for Parkinson’s is a medical history and physical examination conducted by a neurologist.
A neurologist will make a diagnosis based on:
- A detailed history of symptoms, existing medical conditions, current and past medications, family history, and lifestyle factors. Certain medical conditions, as well as some medications, can cause symptoms similar to Parkinson’s.
- A detailed neurological examination during which a neurologist will ask you to perform tasks to assess the agility of arms and legs, muscle tone, gait and balance, to see if:
- Expression and speech are animated
- Tremor can be observed in your extremities at rest or in action
- There is stiffness in your extremities or neck
- There are changes to your walking, step size, and ability to turn
- You can maintain your balance and examine your posture
You may notice that a neurologist records your exam according to the Unified Parkinson’s Disease Rating Scale (UPDRS). This is a universal scale used by neurologists and movement disorder specialists to comprehensively assess and document the exam of a person with PD. This scale can be used as a baseline, to judge the effect of medication, and to track the progression of the disease during future visits.
In Parkinson’s disease, there is a loss of neurons that make the neurotransmitter dopamine. Your doctor may start a medication to help replace dopamine or increase its effect in the brain. These medications are known as dopaminergic medications. Most commonly, people with PD will see improvement in the speed of their movement, stiffness, or tremor when they start dopaminergic medications.
Lack of response to medications may prompt the doctor to seek an alternative diagnosis and order further testing such as an MRI of the brain or lab work. When unsure of a PD diagnosis, a DaTscan can also be considered but is not needed in all cases.
What is a DaTscan and what role does it play in a Parkinson’s diagnosis?
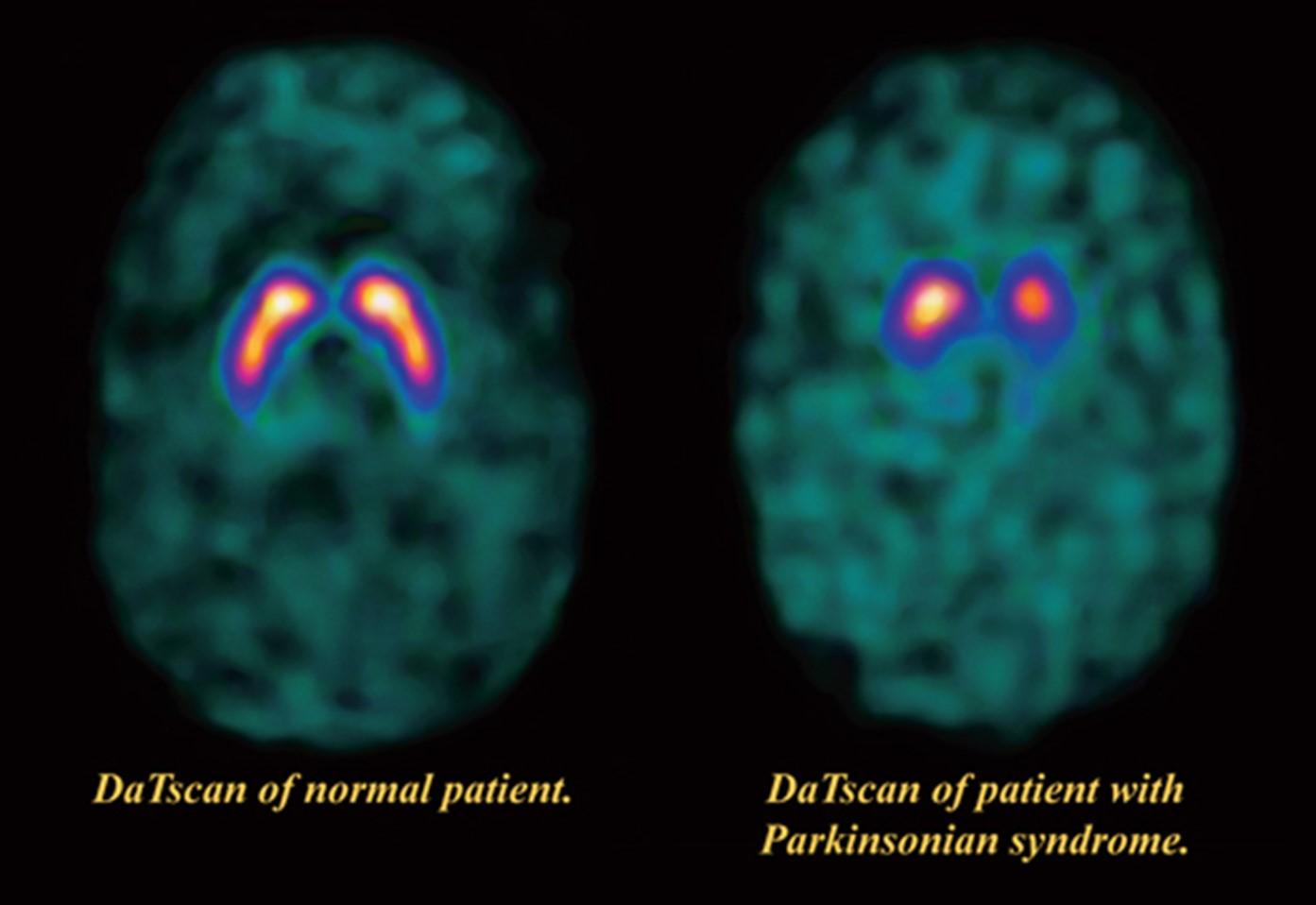
In 2011, the FDA approved the use of a scan called a dopamine transporter scan (DaTscan). A DaTscan is an imaging technology that allows visualization of the dopamine system in the brain. It is similar to an MRI, but instead of looking at the structure of the brain it looks at the function. A DaTscan can show if there is reduced function of the dopamine system in an area of the brain involved in controlling movement.
A DaTscan involves injection of a small amount of a radioactive drug that is then measured by a single-photon emission computed tomography scanner (SPECT scanner). The SPECT scanner measures the levels and location of the drug in the brain.
A negative DaTscan suggests that a person does not have Parkinson’s. It is important to know that a negative DaTscan does not rule out PD, especially early in the disease, but a positive DaTscan can help confirm it. A positive DaTscan can differentiate PD from essential tremor (ET) as there is no dopamine deficiency in the latter. However, DaTscan abnormalities can be seen in PD as well as other forms of atypical parkinsonism that cause a loss of dopamine (Progressive Supranuclear Palsy, Multiple System Atrophy, Corticobasal Syndrome). This means that a positive result does not differentiate Parkinson’s disease from other forms of atypical parkinsonism.
I have PD and several symptoms. Should I get a DaTscan?
In many cases, a DaTscan is not needed to diagnose Parkinson’s disease. There is no need for DaTscan when your history and exam are typical for Parkinson’s disease and you meet the diagnostic criteria. Occasionally, if signs and symptoms are mild or you don’t meet the diagnostic criteria, your doctor will refer you for a DaT scan.
Another reason physicians may order a DaTscan may be to help inform their diagnosis of Parkinson’s disease if you have an unsatisfying response to therapy. Keep in mind that ultimately the diagnosis is based on your history and physical exam. The DaT scan is most commonly used to complete the picture and is not a test for a diagnosis.
There is no need for DaTscan when your history and exam suggest Parkinson’s disease and you meet the diagnostic criteria. Occasionally, if signs and symptoms are mild or you don’t meet the diagnostic criteria, your doctor will refer you for a DaT scan. Keep in mind that ultimately the diagnosis is based on your history and physical exam. The DaT scan is most commonly used to complete the picture and is not a test for a diagnosis.
The Syn-One (Skin Biopsy) Test
The Syn-One Test® is a pathological test that uses a skin sample to confirm the presence of phosphorylation in nerves, which can carry the protein that plays an essential role in Parkinson’s. Test results can help PD doctors confirm a Parkinson’s diagnosis.
For this test, your neurologist, or another physician, will perform three small skin biopsies on the upper back, lower thigh and lower leg. The areas are numbed with a local anesthetic. Results take about two to three weeks to be delivered to your doctor.
CND Life Sciences manufactures this test, processes the tests, and states that Medicare covers the cost of the test when appropriately ordered.
Parkinson's Foundation Helpline
Contact our Helpline at 1-800-4PD-INFO (1-800-473-4636) or Helpline@Parkinson.org for answers to your Parkinson’s questions. Helpline specialists can assist you in English or Spanish, Monday through Friday, 9 a.m. to 7 p.m. ET.
Page reviewed by Dr. Michael S. Okun, Chair of Neurology and Executive Director at the Norman Fixel Institute for Neurological Diseases at the University of Florida Health and Dr. Lauren Fanty, Movement Disorders Fellow at the University of Florida, a Parkinson’s Foundation Center of Excellence.